Meet Audra!

We are excited to introduce you to Audra Geyer, our newest birth doula! She was a recent HypnoBirthing student and birth client of ours who loved the experience so much she decided to become a doula herself! What did you do before you became a doula? I currently work as a Speech Language Pathologist at […]
Meet Savannah!

Meet Savannah Tallman, our newest birth doula! What did you do before you became a doula? Before obtaining my doula education, I was a full time student at Hope College in Holland. There I was able to graduate with a Bachelor of Arts in Exercise Science and Psychology. After graduation I moved to Grand Rapids […]
Acupuncture for Anxiety: Podcast Episode #105
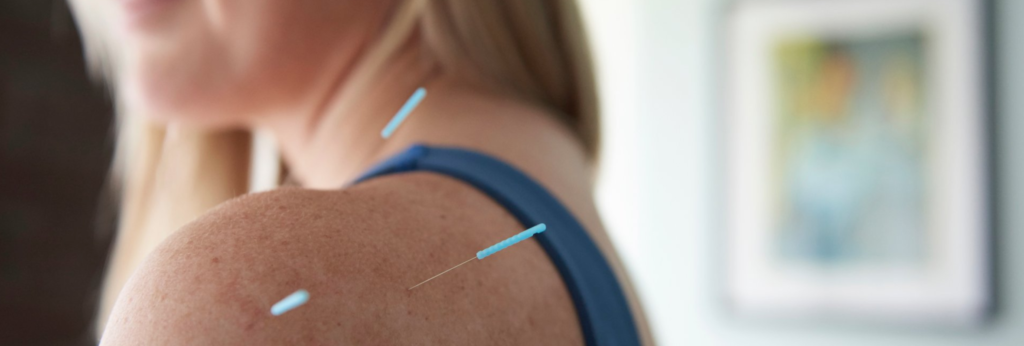
Kristin Revere, Co-Owner of Gold Coast Doulas talks with Vikki Nestico of Grand Wellness about acupuncture to help relieve stress, tension, and anxiety. You can listen to this complete podcast episode on iTunes or SoundCloud. Kristin: Welcome to Ask the Doulas with Gold Coast Doulas. I’m Kristin, and I’m here today with Vikki from […]
What I Wish I Knew: Podcast Episode #104

Kristin and Alyssa, owners of Gold Coast Doulas, talk about the things they wish they had known before having a baby. Listen to this fun episode packed with advice and lots of little gold nuggets of information for new parents! You can listen to this complete podcast episode on iTunes or SoundCloud. Kristin: Welcome to […]
Gold Coast Doulas 5th Annual Diaper Drive

Gold Coast Doulas LLC is holding our 5th annual Diaper Drive from September 1st to October 1st, 2020. Giving back is an important foundation of our business as a Certified B Corporation; clean diapers make a huge impact on the health of new families. Diaper need is something that goes almost completely unrecognized, but 1 […]
Acupuncture during Pregnancy and Postpartum: Podcast Episode #103

Dr. Carrie Dennie, ND speaks with Alyssa about the benefits of acupuncture during pregnancy and postpartum. You can listen to this complete podcast episode on iTunes or SoundCloud. Alyssa: Welcome to the Ask the Doulas Podcast. You are listening to Alyssa Veneklase. I am the co-owner of Gold Coast Doulas, and today, I am […]
Meet Jessi!

Meet our newest Birth Doula, Jessi Heins! She filled out our questionnaire, so let’s get to know her! What did you do before you became a doula? Currently I work part time at a hotel in Douglas, Michigan. Prior to that I was a stay at home parent. I have also made lattes and worked […]
Top 5 Return To Learning Tips

Fall is almost upon us…chunky sweatshirts and boots, falling leaves and school…let’s take a look at how best to prepare mentally and physically for what returning to learning means to you and your family. First of all, you are NOT alone in your feelings of anxiety or vulnerability and it is exhausting living in the land of uncertainty. There are, however, a […]
Saturday Series of Classes: Podcast Episode #102

Kristin Revere, Kelly Emery, and Alyssa Veneklase talk about their Saturday Series of classes offered through Gold Coast Doulas. Each goes in to detail about what their classes cover including Comfort Measures for Labor, Breastfeeding, and Newborn Survival. You can listen to this complete podcast episode on iTunes or SoundCloud. Kristin: Welcome to Ask […]
Creating a Safe Sleep Space: Routers

Alyssa Veneklase talks with Lisa Tiedt, Building Biologist and owner of Well Abode, about creating health sanctuaries in our homes. You can watch this video on YouTube. Alyssa: Hi. It’s Alyssa and Lisa here again. This is Part 3 of our series on how to create a low EMF sleep space, and we’ve kind […]
Creating a Low EMF Sleep Space: Baby Monitors

Alyssa Veneklase talks with Lisa Tiedt, Building Biologist and owner of Well Abode, about creating health sanctuaries in our own homes. You can watch this video on YouTube. Alyssa: Hi, again. We are in our series of how to create a safe sleep space, and I am Alyssa, talking to Lisa Tiedt again. She […]
Creating a Safe Sleep Space: Sound Machines

Alyssa Veneklase talks with Lisa Tiedt, Building Biologist and owner of Well Abode, about creating health sanctuaries in our homes. You can view this video on YouTube. Alyssa: All right. Today, I’m here talking to Lisa Tiedt. She’s a Building Biologist, and, as you know, I’m a sleep consultant, so we’ve partnered a few […]
Fertility and Acupuncture: Podcast Episode #101

Today Kristin talks to Vikki Nestico, R.Ac of Grand Wellness Acupuncture. We learn a lot about fertility and how acupuncture supports the nervous system, reduces stress, and increases blood flow to the reproductive organs. You can listen to this complete podcast episode on iTunes or SoundCloud. Kristin: Hi, Vikki! Vikki: Hi, how are you? […]
Signs of Early Pregnancy
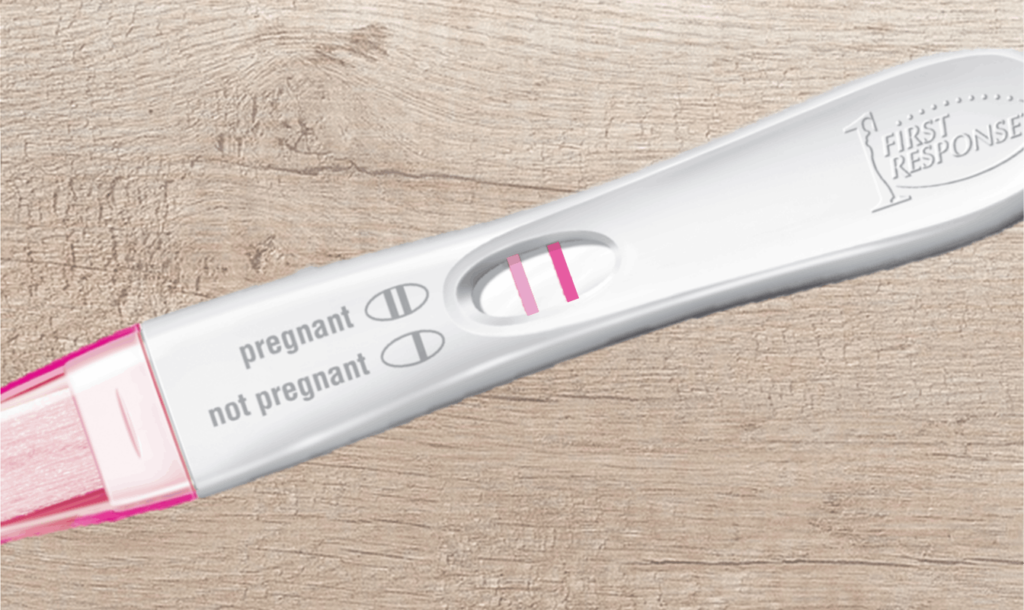
This blog is written by Jessica Kupres, BSN, RN, CLC, CBE a Postpartum Doula with Gold Coast. As you lie in bed thinking about your day and putting your brain to rest, you might think about the great presentation you gave today. Did you put the clothes in the dryer? When was your last period?…. […]
Podcast Episode 100!

It’s the 100th episode! Alyssa and Kristin, co-Owners of Gold Coast Doulas, talk about what the past two and a half years of podcasting has looked like, how the podcast has changed, how the business has changed, how services have pivoted in the midst of the COVID-19 pandemic, and how they are playing their part […]
Hyperemesis Gravidarum
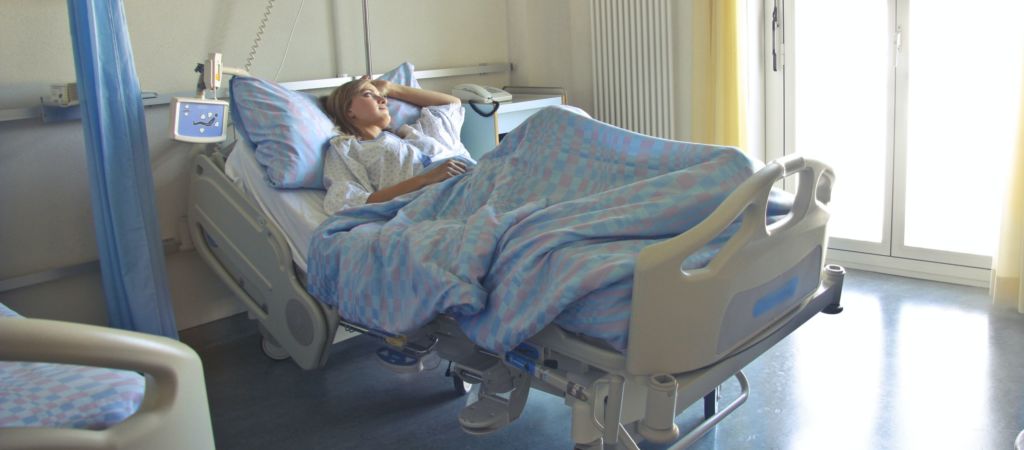
This post was written by Lauren Utter, a ProDoula trained Birth and Postpartum Doula with Gold Coast Doulas. Finding out you are pregnant can bring an array of emotions – planned pregnancy or not. Maybe you’re excited because you have been waiting for this day. Maybe you are surprised because a baby wasn’t on your […]
Adult Separation Anxiety: Podcast Episode #99
On this episode, Alyssa and Laine begin by talking about parenting anxiety and the distance that parents can sometimes feel as their babies and children grow and seem to need them less. The conversation takes some interesting turns to talk about having clear boundaries for kids, pivoting our expectations of children as they grow, and […]
My Favorite Sleep Products

During sleep consultations I am often asked what my favorite products are. While I have many, parents must realize that my favorite sleep sack or swaddle may not be their child’s favorite! I will list several products in this blog and tell you why I like them, but you know your baby or child best. […]
Top 10 New Parent Essentials

Did you notice that this list doesn’t say “Baby Essentials”? Nope, it’s not an error. YOU are the single most essential thing in your baby’s tiny life. While you process all the feels over this game changing reality, I’ve got your back with some advice on essentials that will ease your transition so that you […]
Parenting and Sleep: Podcast Episode #98

Laine Lipsky, Parenting Coach, talks with Alyssa today about the negative effects of sleep deprivation on children and parents. You can listen to this complete podcast episode on iTunes or SoundCloud. Alyssa: Hello and welcome to the Ask the Doulas Podcast. I am Alyssa Veneklase. I’m excited to be back with Laine Lipsky, parenting coach. […]
Mental Health Awareness Month: Podcast Episode #97

Dr. Nave now works with queens through her virtual practice Hormonal Balance. Today she talks to us about hormones and how they affect our mental health, including the baby blues and postpartum depression. You can listen to this complete podcast episode on iTunes or SoundCloud. Alyssa: Hi. Welcome to Ask the Doulas Podcast. I am […]
Parenting During Covid-19: Podcast Episode #96

Today we talk with Laine Lipsky, parenting coach, about some best practices for parenting during the COVID-19 pandemic. She gives us all some great tips on how to manage stress and deal with out children no matter what age! You can listen to this complete podcast episode on iTunes or SoundCloud. Alyssa: Hello and welcome […]
Planning a Nursery During the COVID-19 Pandemic

Today’s guest blog is written by Isabella Caprario, Content Marketing Specialist at Porch. During the COVID-19 pandemic, we all feel uncertainty. We don’t know what will happen or what steps to take next. We only know that the best way to end this madness is to sit at home and take all the necessary precautions […]
Virtual Birth Support: Podcast Episode #95

Sam & Justin recently had their baby boy, Judah, in the hospital in the midst of the COVID-19 pandemic. They describe their experience in the hospital as well as how beneficial birth doula support was throughout pregnancy and then during labor and delivery, even though support was virtual instead of in-person. You can listen to […]


