Don’t be scared of pelvic floor physical therapy! Podcast episode #117

Amanda and Katie, women’s health physical therapists at Hulst Jepsen Physical Therapy, give us an intro into pelvic floor PT. What is it, what does an internal vs external pelvic floor exam involve, and what kinds of symptoms can pelvic floor PT treat? You can listen to this complete podcast episode on iTunes or SoundCloud. […]
Meet Lee Ann, our newest birth & postpartum doula!

What did you do before you became a doula? Currently, I own my own Health & Wellness business through Isagenix. In addition, I work as an Interior Designer for a company that does home staging for realtors and their clients. Previously I was an Administrative Assistant for Leadership Events throughout the US and Canada. What […]
Meet Jessica Moeckel, RN – our newest Birth & Postpartum Doula!

What did you do before you became a doula? I was a RN at Mary FreeBed, then I transitioned to Saint Mary’s L&D. Most recently, I was at Mercy Health Physician Partners. What inspired you to become a doula? The first birth I attended was in college during the L&D portion of nursing school. In […]
2020 Year in Review

Although 2020 threw us a curveball, we still had a great year. We supported more clients than ever and worked diligently to find ways to support them safely. Here are some of our accomplishments. Worked with 218 clients. Attended 81 births. Worked 2,900 postpartum hours. Supported 10 twin and triplet families. Had 22 lactation visits. […]
Keeping Yourself Healthy During Pregnancy: Podcast Episode #116

Kristin talks with Dr. Annie of Rise Wellness Chiropractic about how to keep yourself and your family healthy during pregnancy and a pandemic! You can listen to this complete podcast episode on iTunes or SoundCloud. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over the country about […]
Real Food for Gestational Diabetes: Podcast Episode #115

Author Lily Nichols talks to Kristin about gestational diabetes during pregnancy and how eating has such a profound impact on our health and energy levels. You can listen to this complete podcast episode on iTunes or SoundCloud. Be sure to check out Lily’s book! Welcome. You’re listening to Ask the Doulas, a podcast where we […]
Creating a Calm Space: Podcast Episode #114

Today Amber Brant of The Coziness Consultant talks with Alyssa about how new moms can create a calm space in their homes in the midst of chaos. You can listen to this complete podcast episode on iTunes or SoundCloud. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all […]
Preparing your dog for a new baby: podcast episode #113

Today Kristin talks to Jenn Gavin, owner of A Pleasant Dog in Grand Rapids, MI about when to prepare your dogs for the arrival of a new baby. You can listen to this complete podcast episode on iTunes or SoundCloud. Alyssa: Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts […]
Birthing in a Pandemic
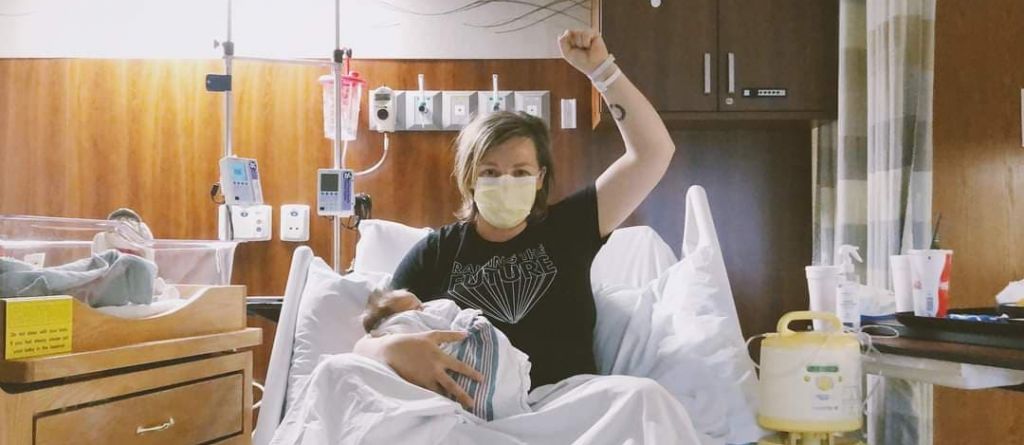
We have seen so much strength and resilience from our clients and our subcontracted doulas within the last year. Being pregnant and birthing in a pandemic is no joke. Gold Coast has supported over 200 families during this time. We are so thankful for the trust they placed in us. Our birth doulas have worked […]
Bebcare Low EMF Baby Monitors: Podcast Episode #112

Baby monitors: Today Alyssa, a sleep consultant at Gold Coast Doulas, speaks with Lisa, a Building Biologist at Well Abode, and Brian, an engineer at Bebcare. Bebcare has the lowest EMF baby monitors on the market. The conversation gets a little technical but it’s really interesting, and you may learn a thing or two about […]
Meet Jaclyn!

Meet Jaclyn Geroux, our newest postpartum doula! She filled out our questionnaire, so let’s get to know her! What did you do before you became a doula? I’ve spent the last 3.5 years as a stay at home mom. Prior to that, I was employed as an advocate for individuals with intellectual and developmental disabilities, […]
Transformed by Postpartum Depression: Podcast Episode #110
Alyssa: Hi. Welcome to the Ask the Doulas Podcast. My name is Alyssa Veneklase. I am co‑owner of Gold Coast Doulas, and today, I have Jessica Kupres, one of our postpartum doulas, with us, and we are both so excited to talk to Dr. Ladd. She is the author of a book called […]
Bebcare – A safe monitor for your baby’s nursery

A while ago I recorded three videos about electromagnetic emissions and creating a sleep sanctuary for your child. You can find all three on our YouTube channel. I spoke with Lisa Tiedt, a Building Biologist at Well Abode. She used science to physically demonstrate to us how baby monitors, sound machines, and wifi modems emit […]
Car Seat Safety with Secure Quest: Podcast Episode #109

Kristin talks with Jennifer Hoekstra, one of the owners of Secure Quest, about car seat safety for our babies and toddlers. You’ll be astonished at how many of us install our car seats incorrectly! You can listen to this complete podcast episode on iTunes or SoundCloud. Kristin: Welcome to Ask the Doulas with Gold […]
Meet Ashley Harland!

Meet Ashley Harland, our newest postpartum doula! 1) What did you do before you became a doula? Before I became a doula I did many things! I’ve done photography (and still do), started an eco-friendly farm, homeschooled my children, did housekeeping, and mentored special needs adults to name a few! 2) What inspired you to […]
What I Didn’t Know About Pregnancy and Birth: Podcast Episode #107

Today Kristin and Alyssa talk about some interesting, and funny, and gross things that happened to their bodies during pregnancy and birth that were a bit unexpected! You can listen to this complete podcast episode on iTunes or SoundCloud. Alyssa: Hi and welcome to the Ask the Doulas podcast. I am Alyssa Veneklase, […]
Sleep and Virtual School: Podcast Episode #106

Kristin and Alyssa talk about the struggle to get kids to sleep during virtual school at home. Is it important to have a set bedtime? Can kids stay up late? We answer these questions and more! You can listen to this complete podcast episode on iTunes or SoundCloud. Alyssa: Hello. Welcome to the Ask […]
Audra’s Birth Story: Podcast Episode #105

Audra Geyer, Gold Coast’s newest birth doula, tells us her birth story and how birth support from her doula was a game changer. She also took HypnoBirthing classes and went from being afraid of labor to looking forward to it! Her experience with Gold Coast let her to become a doula herself! You can […]
Meet Audra!

We are excited to introduce you to Audra Geyer, our newest birth doula! She was a recent HypnoBirthing student and birth client of ours who loved the experience so much she decided to become a doula herself! What did you do before you became a doula? I currently work as a Speech Language Pathologist at […]
Meet Savannah!

Meet Savannah Tallman, our newest birth doula! What did you do before you became a doula? Before obtaining my doula education, I was a full time student at Hope College in Holland. There I was able to graduate with a Bachelor of Arts in Exercise Science and Psychology. After graduation I moved to Grand Rapids […]
Acupuncture for Anxiety: Podcast Episode #105
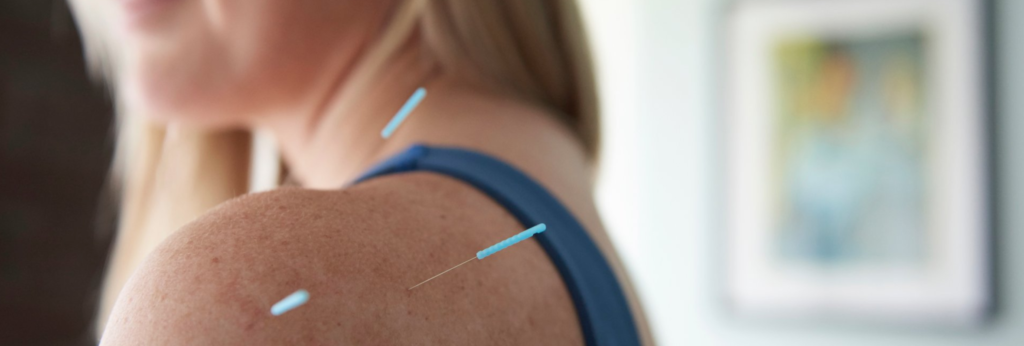
Kristin Revere, Co-Owner of Gold Coast Doulas talks with Vikki Nestico of Grand Wellness about acupuncture to help relieve stress, tension, and anxiety. You can listen to this complete podcast episode on iTunes or SoundCloud. Kristin: Welcome to Ask the Doulas with Gold Coast Doulas. I’m Kristin, and I’m here today with Vikki from […]
What I Wish I Knew: Podcast Episode #104

Kristin and Alyssa, owners of Gold Coast Doulas, talk about the things they wish they had known before having a baby. Listen to this fun episode packed with advice and lots of little gold nuggets of information for new parents! You can listen to this complete podcast episode on iTunes or SoundCloud. Kristin: Welcome to […]
Gold Coast Doulas 5th Annual Diaper Drive

Gold Coast Doulas LLC is holding our 5th annual Diaper Drive from September 1st to October 1st, 2020. Giving back is an important foundation of our business as a Certified B Corporation; clean diapers make a huge impact on the health of new families. Diaper need is something that goes almost completely unrecognized, but 1 […]
Acupuncture during Pregnancy and Postpartum: Podcast Episode #103

Dr. Carrie Dennie, ND speaks with Alyssa about the benefits of acupuncture during pregnancy and postpartum. You can listen to this complete podcast episode on iTunes or SoundCloud. Alyssa: Welcome to the Ask the Doulas Podcast. You are listening to Alyssa Veneklase. I am the co-owner of Gold Coast Doulas, and today, I am […]


