Podcast Episode #23: Amber’s Cesarean Birth Story

On this episode of Ask the Doulas, Amber shares how her Gold Coast Doulas supported her through her C-section experience. You can listen to this complete episode on iTunes and SoundCloud. Alyssa: Hi, welcome to another episode of Ask the Doulas. I am Alyssa Veneklase, co-owner and postpartum doula, and we are talking to […]
Podcast Episode #22: How to get Dad on board with Hiring a Doula

On this episode of Ask the Doulas, Alyssa talks with Amber and Ashton about getting your husband or partner on board with hiring a doula. You can listen to this complete podcast on iTunes or Soundcloud. Alyssa: Hi, welcome to another episode of Ask the Doulas. I am Alyssa Veneklase, co-owner and postpartum doula, […]
Podcast Episode #21: Supporting a Cesarean Birth
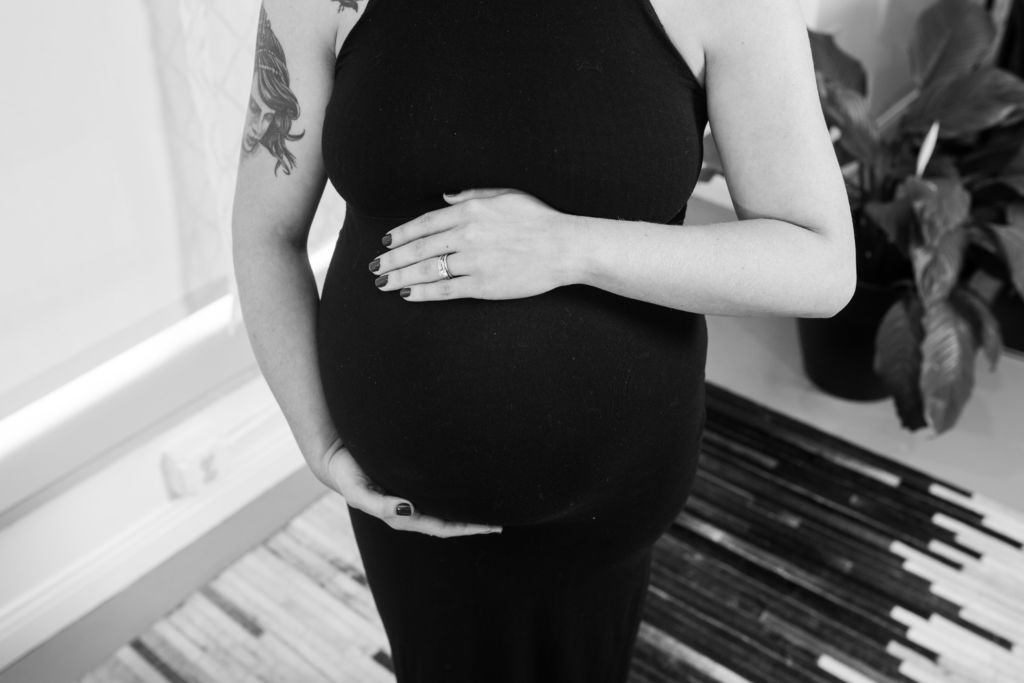
April is C-section Awareness Month! On this episode of Ask the Doulas, Alyssa and Ashley talk about how birth doulas provide support during a Cesarean section delivery. You can listen to the full podcast episode on iTunes or Soundcloud. Alyssa: Hi, welcome to Ask the Doulas with Gold Coast Doulas. I am Alyssa, co-owner […]
Podcast Episode #20: Lisa’s Story about Postpartum Anxiety
On this episode of Ask the Doulas, Lisa shares about her postpartum experience of dealing with anxiety and how doula support helped her through that challenging time. You can listen to the complete podcast on iTunes and Soundcloud. Please also visit our postpartum depression and anxiety resource list. Alyssa: Hi, welcome back to Ask the […]
Podcast Episode #19: Lisa’s Postpartum Journey

On this episode of Ask the Doulas, Alyssa talks with Lisa about her postpartum doula and how having a doula helped with her recovery. You can listen to the complete podcast on iTunes and SoundCloud. Alyssa: Hi, welcome to another episode of Ask the Doulas with Gold Coast Doulas. I am Alyssa Veneklase. […]
World Doula Week 2018

Today’s blog is written by Kristin Revere, Certified Birth and Postpartum Doula and Certified Sacred Postpartum Mother Roaster. As the end of World Doula Week nears, I feel I must speak my truth. Before having kids my purpose was to support women in politics. I wanted more voices in office and wanted to run for […]
Podcast Episode #17: How to Find a Babysitter You Trust

On this episode of Ask the Doulas, Alyssa and Cindy talk about how to find a babysitter that you trust to watch your kids. You can listen to this entire podcast epidode on iTunes and Soundclound. Alyssa: Hi, welcome to another episode of Ask the Doulas. I am Alyssa, and I’m here with Cindy from […]
Make Your Hospital Room Feel Like Home

Today’s blog comes from one of our past birth doulas, Courtney Garvelink. Her experience with birth clients, as well as being a licensed massage therapist and previous HypnoBirthing instructor, makes her an expert on comfort measures in the delivery room. See what she has to say about making your hospital birth feel more like home. […]
Postpartum Depression & Anxiety Resource List

After our recent event at the Wealthy Street Theatre where we screened ‘When the Bough Breaks – A Documentary about Postpartum Depression’ we realized that there are many great resources available to our community, but people may not know how to find them. We at Gold Coast, with the help of Cristina Stauffer, have compiled […]
The Modern Grandparent

Understanding the Modern Parent First of all congratulations on becoming a Grandparent! Whether this is your 1st or 5th, it is a very excited time for the whole family. Gold Coast Doulas offers in-home private classes for The Modern Grandparent. We are not currently offering group classes. This 2 ½ hour class will break down […]
Mom Guilt: How to Survive it and Grow from it

Today’s guest blogger is a past birth client of ours, Nicole Vega, LMSW, CHC. Nicole is a fully licensed clinician and certified health coach. Nicole received her Master’s in Clinical Social Work in 2012 from Western Michigan University and became certified as a health coach in 2016. Her work is founded on the principle that individuals […]
Meet our new birth doula, Angel!

1) What did you do before you became a doula? I have been a stay at home mom for the past (almost) four years. Before that I worked as a medical assistant in a few different areas, end of life care and a neurosurgeons office. 2) What inspired you to become a doula? I was […]
What does non-judgmental support mean?

Author: Alyssa Veneklase, CD I was recently asked if, since I’m a doula, I tell clients not to vaccinate and make them feel guilty if they don’t breastfeed. What??! If you had a doula that made you feel this way, I apologize on behalf of them. That is the opposite of what a doula […]

